 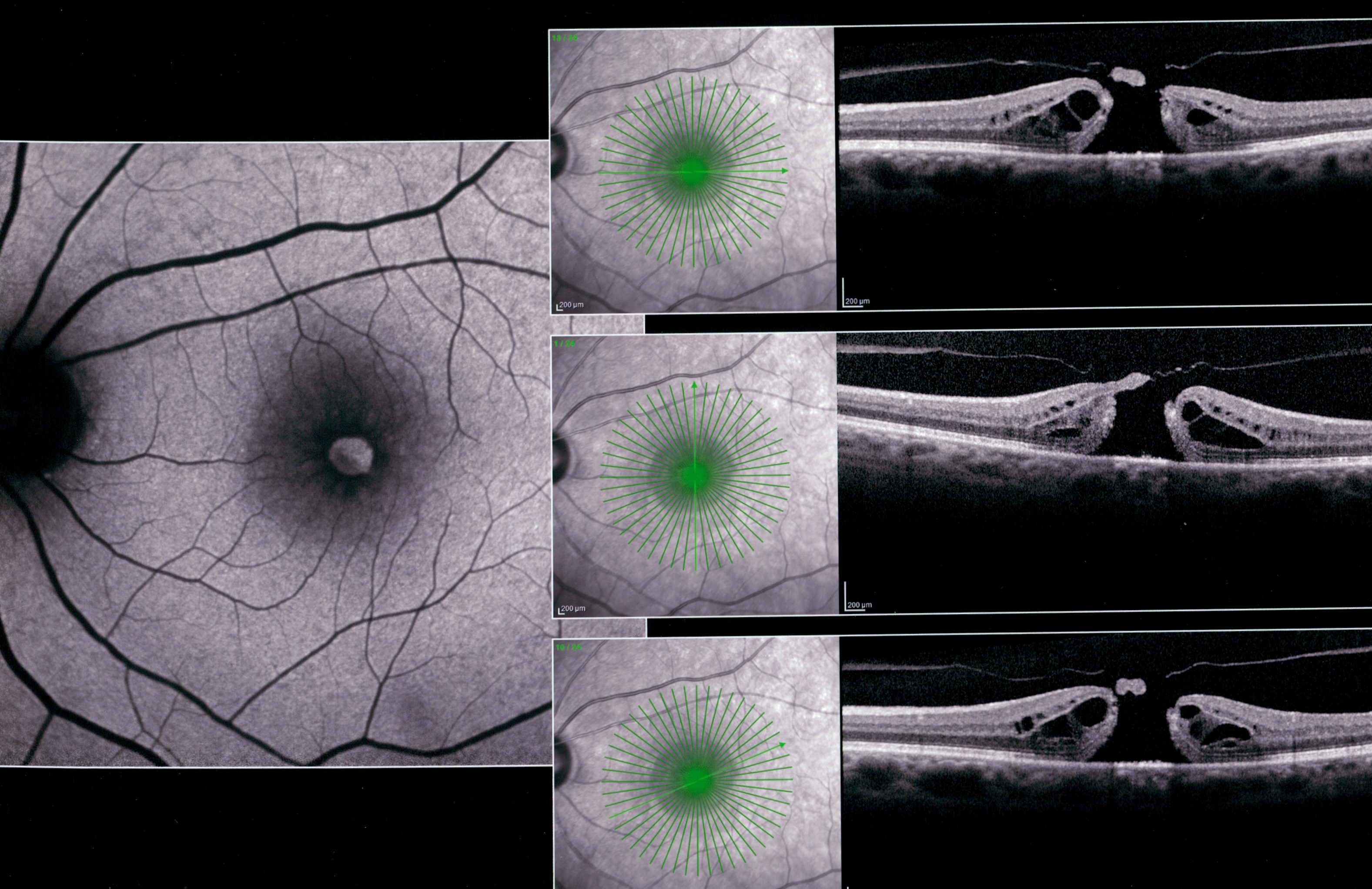
If the posterior vitreous detaches from the optic disc and macula, a stage 3 macular hole becomes a stage 4 macular hole. Stage 2 macular holes enlarge and become stage 3 macular holes when they reach a diameter of approximately 400 microns in size. Stage 2 macular holes can be central (with or without a pre-foveolar opacity) or eccentric with a crescent or horseshoe shape break at the edge of the yellow ring. Progression to stage 2, or full thickness macular hole, has been reported to occur about fifty percent of the time. Stage 1B appears as a yellow ring that is believed to represent centrifugal displacement of the foveolar retina and xanthophyll pigment. Stage 1A has loss of the foveolar depression with a central yellow spot. They divided the initial stage into stage 1A, impending macular hole, and stage 1B, an occult hole. Gass and Johnson were the first to classify idiopathic macular holes into four stages using very keen biomicroscopic observations. Morphing videos from serial OCTs are a useful tool and helped illustrate and support anterior-posterior vitreofoveal traction with subsequent retinal hydration as the pathogenesis of idiopathic macular holes. Surgical repair of a macular hole revealed initial closure of the macular hole with subsequent reabsorption of the sub-retinal fluid and restoration of the foveal contour. During cyst formation, the macular hole enlarged as the edges of the hole became elevated from the retinal pigment epithelium (RPE) with an increase in subretinal fluid. Progression of the macular hole occurred with increased cystic thickening of the fovea without evidence of further vitreofoveal traction. The videos supported anterior-posterior vitreofoveal traction as the initial event in macular hole formation. Morphing videos from serial OCTs allowed the OCTs to be viewed dynamically. Images centered at the fovea and at the same orientation were digitally exported and morphed into an Audiovisual Interleaving (avi) movie format. Two patients at the onset of symptoms with early stage macular holes and one patient following repair were followed with serial OCTs. Treatment works best when doctors catch macular holes early, so it’s important to talk to your eye doctor right away if you notice symptoms of a macular hole.To use a new medium to dynamically visualize serial optical coherence tomography (OCT) scans in order to illustrate and elucidate the pathogenesis of idiopathic macular hole formation, progression, and surgical closure. You also need to avoid flying or getting nitrous oxide (laughing gas) for any procedures until the bubble is completely gone - these things can affect the pressure in your eye. It can be hard to limit your head movement, so talk to your doctor about how you can best recover from a vitrectomy. This keeps the bubble in the right place so the macular hole can heal. The bubble is like a temporary bandage that holds the edges of the macular hole together and helps your eye close the hole.Īfter the surgery, you’ll need to limit your activities and movement for a while. If a macular hole is affecting your vision, you’ll probably need a type of surgery called vitrectomy to fix the hole and prevent permanent vision loss.ĭuring a vitrectomy, the doctor removes the vitreous and some tissues on the surface of the macula and injects a gas bubble into your eye. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
